What Is the Retina?
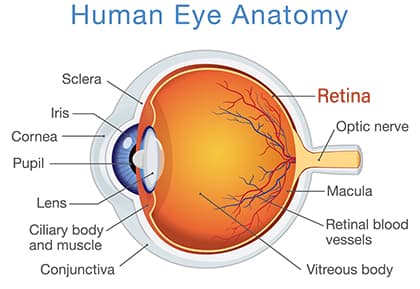 The retina is a thin layer of nerve cells located at the back of the eye. A healthy retina is essential for good vision.
The retina is a thin layer of nerve cells located at the back of the eye. A healthy retina is essential for good vision.
When light enters the cornea and lens, retinal photoreceptor cells convert it into electrical impulses. The optic nerve sends these impulses to the brain.
These impulses are then converted into images and visual perceptions.
How Does the Retina System Work?
The retina is made up of several important parts. A disease or problem in any of these areas can cause vision loss:
- Macula – allows us to see detailed images clearly.
- Fovea -an area in the center part of the macula that affects visual clarity
- Peripheral Retina – enables side vision and night vision.
- Photoreceptors -cells that convert light into impulses sent to the brain. Rods give us night vision, and cones enable our color vision.
Is Retinal Disease Preventable?
There are many retina diseases and conditions. Not all retina diseases and conditions are preventable. There are treatments available. These help patients keep as much vision as possible.
Early treatment can be critical when managing retinal disease. Any patient who is at risk for retina problems should have regular dilated eye exams.
The same is true if you have already gotten diagnosed with a retinal disease. Regular dilated eye exams and follow-up appointments with an ophthalmologist are crucial!
Here are some of the more common retinal diseases and conditions:
Age-Related Macular Degeneration (AMD or ARMD)
AMD is an eye disease that involves the deterioration of the macula and choroid. It is the leading cause of loss of visual acuity in people over 50.
Macular degeneration does not cause total blindness, but it can be very debilitating.
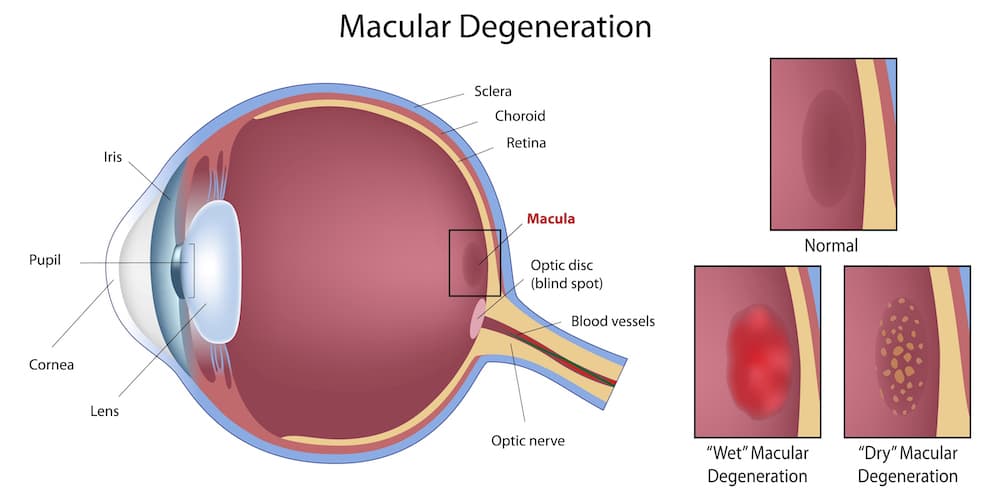
There are two types of macular degeneration (AMD). In later stages, both types involve loss of central vision. This affects the ability to read, drive, recognize faces, and do close work.
Dry AMD (also known as non-neovascular AMD) is more common, and often develops slowly. Areas of atrophy or wasting may occur in the retina.
Sometimes it progresses into wet AMD. Scientists believe that maintaining a healthy lifestyle, may slow its progression. This includes good nutrition, exercise, and not smoking.
Wet AMD (also known as neovascular AMD) is a disease where abnormal blood vessels grow beneath the retina. They can bleed or leak, which causes swelling and damage to the macula.
Symptoms can occur suddenly and cause noticeable vision damage.
Are There Treatments for AMD?
If you are diagnosed with AMD, your ophthalmologist may order advanced testing. This helps determine the best treatment.
Not all cases of macular degeneration progress to serious loss of vision.
Timely treatment can often reduce severe vision loss. Patients are often encouraged to use an Amsler grid. This is a handheld chart showing line distortion at home to track vision changes.
If you notice significant changes, let your doctor know as soon as possible.
- Laser treatments can benefit some patients.
- There is no proven treatment for late stage dry AMD.
- Intravitreal injections – The injection of anti-VEGF (vascular endothelial growth factor) drugs into the vitreous gel inside the eye can be a highly effective treatment for advanced wet AMD.
These drugs stop the growth of new blood vessels in the eye. Most patients need a series of injections.
Diabetic Retinopathy
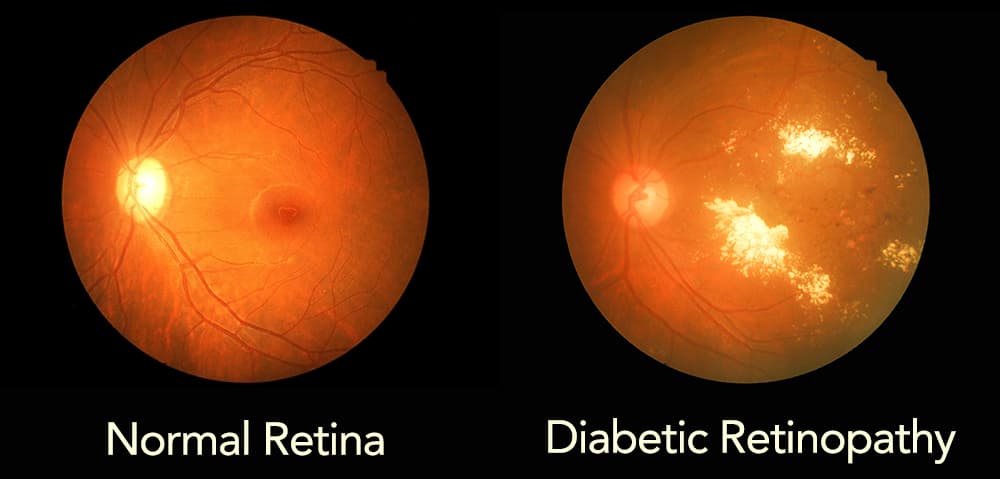
This condition affects the blood vessels in the retina. In early stages, vision loss can be reduced with proper medical management. It can lead to severe vision loss and blindness if the disease is not under control.
- Non-proliferative retinopathy (NPDR) is the early stage of the disease. Small areas of swelling occur, and the capillaries (tiny blood vessels) can begin to leak.
- Proliferative retinopathy (PDR) is an advanced stage of retinopathy. New blood vessels grow along the surface of the retina and into the vitreous gel.
This is the fluid that fills the back of the eye. The fragile blood vessels often bleed and leak. Retinal detachment is a dangerous side effect of PDR.
How is Proliferative Retinopathy Treated?
- Scatter Laser Surgery or Panretinal Photocoagulation helps shrink blood vessels and reduce retina swelling. It involves creating tiny thermal burns in the retina.Unfortunately, the procedure sometimes damages peripheral and night vision while preserving central vision.
- Anti-VEGF Injections- Anti-VEGF injections were originally used for diabetic macular edema. They have recently shown to be useful in earlier stages of retinopathy.
- Vitrectomy Surgery is sometimes recommended for advanced PDR. In this surgery, a retina specialist will remove blood and vitreous gel from the back of the eye. This allows light rays to focus correctly on the retina.
Epiretinal Membrane (ERM)
ERM or Macular Pucker, occurs when a defect in the retina causes semi-translucent membranes to form inside the retina. When the membranes affect the macula, they can cause visual distortion. This visual distortion makes straight shapes appear crooked.
Treatment:
In cases with significant vision loss, vitrectomy surgery is the only recommended treatment.
Macular Edema
Macular edema is a serious condition that can lead to severe vision loss and blindness. There are many underlying causes. These include diabetes, macular degeneration, inflammatory diseases, blood disorders, and eye injuries.
Leaking from damaged blood vessels or growth of new vessels causes the swelling.
Treatment:
The best treatment is treating the underlying cause of the macular edema. For some, this may mean controlling blood sugar levels for diabetics.
Ophthalmologists also use anti-VEGF intravitreal injections. This is as a direct method of controlling excess fluid caused by leaking blood vessels.
Macular Hole
During aging, the vitreous gel often begins to shrink and separate from the retina. If a piece of the vitreous sticks to the macula it can cause a hole to develop.
The major symptom is usually distorted or wavy vision. This is a serious eye problem which can lead to blindness if not treated.
Treatment:
A macular hole diagnosis requires vitrectomy surgery. The surgeon will remove the vitreous that is pulling on the macula, and then put a gas bubble into the eye.
The bubble flattens the macula and holds it in place while the eye heals. The gas bubble dissolves within a few weeks.
What Causes Retinal Detachment?
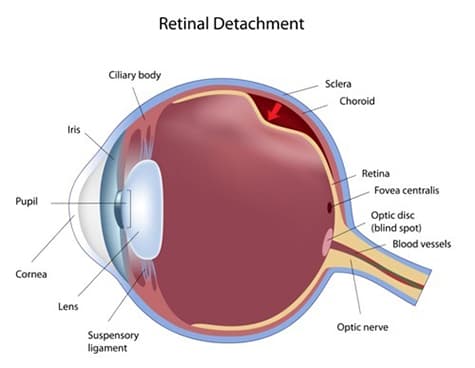 Retinal detachment occurs when the retina detaches from the back of the eye. The retina will not function if it separates from its blood supply. Retinal detachments can occur suddenly. This can be for a variety of reasons, including aging, disease and trauma. Symptoms include:
Retinal detachment occurs when the retina detaches from the back of the eye. The retina will not function if it separates from its blood supply. Retinal detachments can occur suddenly. This can be for a variety of reasons, including aging, disease and trauma. Symptoms include:
- “Floaters” in the eye
- Flashing light
- A shadow on the side of the eye that may progress towards the center of vision.
Treatments:
Retinal detachments are usually an emergency! They must be treated by an ophthalmologist to reduce severe vision loss!
Laser treatments and pneumatic retinopexy (injection of a gas bubble into the eye) can be used for minor detachments. For more serious retinal detachments, vitrectomy or scleral buckle surgeries are necessary.
Have more questions about the retina and how to treat it? Schedule a consultation at Huffman & Huffman, P.S.C. today!

